Auditing Anorectal Manometric Disorders in Children with Constipation at a Hospital in Colombia
DOI:
https://doi.org/10.22516/25007440.1195Keywords:
Constipation, Manometry, Pediatrics, Gastrointestinal motilityAbstract
Introduction and Objectives: Anorectal disorders can be an underlying cause of chronic refractory constipation in pediatric patients. This study aims to identify such disorders using high-resolution anorectal manometry (HRAM) in children with chronic refractory constipation.
Materials and Methods: A retrospective, observational, descriptive cross-sectional data analysis was conducted based on HRAM performed in patients under 18 years old with chronic refractory constipation at a hospital in Colombia between 2014 and 2018. An exploratory descriptive analysis of demographic variables and manometric parameters was performed. Conventional manometric diagnoses were compared and aligned with the London classification.
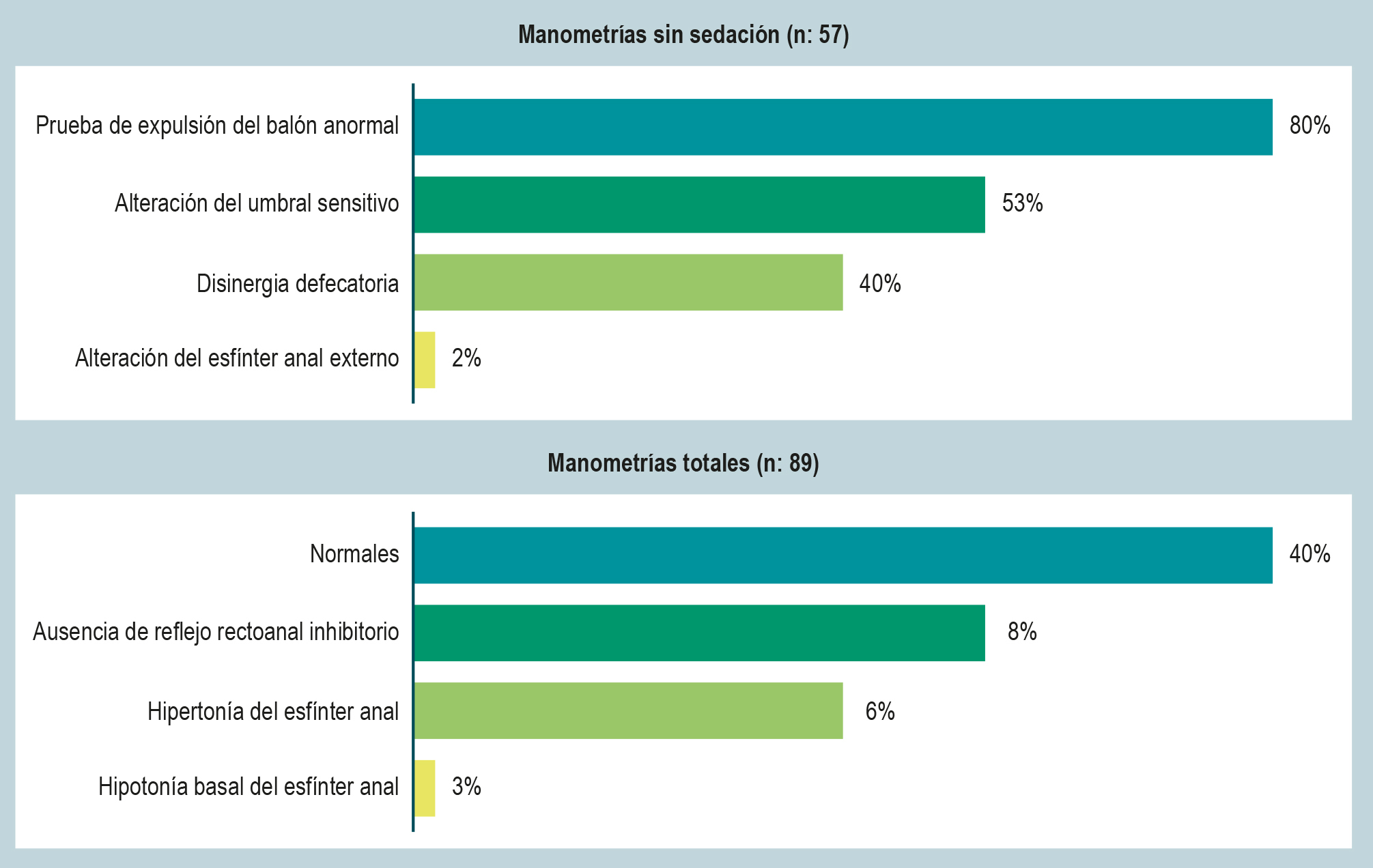
Results: A total of 89 patients were evaluated. According to the conventional classification, 60% of the patients had abnormalities on manometry, and 8% lacked a rectoanal inhibitory reflex (RAIR). HRAM without sedation was performed in 57 patients, of whom 80% showed an abnormal balloon expulsion test (BET); 53% had alterations in sensory thresholds, and 40% exhibited dyssynergic defecation. When extrapolated to the London classification, 93% were found to have rectal sensory disorders; 84% had rectoanal coordination disorders; 39% presented tone and contractility disorders, and 11% had rectoanal areflexia.
Conclusions: Anorectal disorders are common in children with chronic refractory constipation and are diagnosed using HRAM to guide prognosis and targeted treatments, such as for dyssynergias. A classification similar to the London system, with manometric values tailored to pediatric populations by age groups, would provide a systematic and complementary approach to traditional methods and enhance diagnostic sensitivity.
Downloads
References
Koppen IJN, Di Lorenzo C, Saps M, Dinning PG, Yacob D, Levitt MA, et al. Childhood constipation: finally something is moving! Expert Rev Gastroenterol Hepatol. 2016;10(1):141-155. https://doi.org/10.1586/17474124.2016.1098533
Mugie SM, Di Lorenzo C, Benninga MA. Constipation in childhood. Nature Rev Gastroenterol Hepatol. 2011;8(9):502-511. https://doi.org/10.1038/nrgastro.2011.130
Remes Troche JM, Chávez Barrera JA, Worona Dibner LB. Guidelines for diagnosis and treatment of constipation in Mexico. D) Evaluation and treatment of constipation in pediatric population. Rev Gastroenterol Mexico. 2011;76(2):155-168.
Rajindrajith S, Devanarayana NM, Crispus Perera BJ, Benninga MA. Childhood constipation as an emerging public health problem. World J Gastroenterol. 2016;22(30):6864-6875. https://doi.org/10.3748/wjg.v22.i30.6864
Saps M, Nichols-Vinueza DX, Rosen JM, Velasco-Benítez CA. Prevalence of functional gastrointestinal disorders in Colombian school children. J Pediatr. 2014;164(3):542-545.e1. https://doi.org/10.1016/j.jpeds.2013.10.088
Madani S, Tsang L, Kamat D. Constipation in Children: A Practical Review. Pediatr Ann. 2016;45(5):e189-196. https://doi.org/10.3928/00904481-20160323-01
Tabbers MM, DiLorenzo C, Berger MY, Faure C, Langendam MW, Nurko S, et al. Evaluation and treatment of functional constipation in infants and children: evidence-based recommendations from ESPGHAN and NASPGHAN. J Pediatr Gastroenterol Nutr. 2014;58(2):258-274. https://doi.org/10.1097/MPG.0000000000000266
Hasosah M. Chronic refractory constipation in children: think beyond stools. Global Pediatric Health 2021;8:2333794X211048739. https://doi.org/10.1177/2333794X211048739
Tambucci R, Quitadamo P, Thapar N, Zenzeri L, Caldaro T, Staiano A, et al. Diagnostic Tests in Pediatric Constipation. J Pediatr Gastroenterol Nutr. 2018;66(4):e89-e98. https://doi.org/10.1097/MPG.0000000000001874
Athanasakos E, Cleeve S, Thapar N, Lindley K, Perring S, Cronin H, et al. Anorectal manometry in children with defecation disorders BSPGHAN Motility Working Group consensus statement. Neurogastroenterol Motil. 2020;32(6):e13797. https://doi.org/10.1111/nmo.13797
Delgado AF, Barney VAC, de Ardila ACH, Naranjo AML, Hani AFA, Madrid DMM. Actualización con la clasificación de Londres en la interpretación de la manometría anorrectal de alta resolución. Rev Colomb Gastroenterol. 2019;34(4):411-415. https://doi.org/10.22516/25007440.484
Lee YY, Erdogan A, Rao SS. High resolution and high definition anorectal manometry and pressure topography: diagnostic advance or a new kid on the block? Curr Gastroenterol Rep. 2013;15(12):360. https://doi.org/10.1007/s11894-013-0360-2
Rocca A, Chávez JA, Ditaranto A, Falcon AC, Mortarini A, Neder D, et al. Estudios de motilidad en pediatría: aspectos técnicos, indicaciones y limitaciones en los niños. NeuroGastroLatam Rev. 2022;6(3):164-180. https://doi.org/10.24875/NGL.22000022
Rodriguez L, Sood M, Di Lorenzo C, Saps M. An ANMS‐NASPGHAN consensus document on anorectal and colonic manometry in children. Neurogastroenterol Motil. 2017;29(1):e12944. https://doi.org/10.1111/nmo.12944
Banasiuk M, Banaszkiewicz A, Dziekiewicz M, Załęski A, Albrecht P. Values from three-dimensional high-resolution anorectal manometry analysis of children without lower gastrointestinal symptoms. Clin Gastroenterol Hepatol. 2016;14(7):993-1000. https://doi.org/10.1016/j.cgh.2016.01.008
Carrington EV, Heinrich H, Knowles CH, Fox M, Rao S, Altomare DF, et al. The international anorectal physiology working group (IAPWG) recommendations: Standardized testing protocol and the London classification for disorders of anorectal function. Neurogastroenterol Motil. 2020;32(1):e13679. https://doi.org/10.1111/nmo.13679
Dinning PG, Carrington EV, Scott SM. The use of colonic and anorectal high-resolution manometry and its place in clinical work and in research. Neurogastroenterol Motil. 2015;27(12):1693-1708. https://doi.org/10.1111/nmo.12632
Tuduri Limousin I, Cabo Valdés JA, Moya Jiménez MJ, Granero Cendón R, Fernández Pineda I, Cabrera García R, et al. Fiabilidad de la manometría anorrectal para el diagnóstico de la enfermedad de Hirschsprung en neonatos: experiencia de 25 años. Cir Pediátr. 2008;21(4):232-4.
Keshtgar AS, Ward HC, Clayden GS. Pathophysiology of chronic childhood constipation: functional and morphological evaluation by anorectal manometry and endosonography and colonic transit study. J Pediatr Surg. 2013;48(4):806-812. https://doi.org/10.1016/j.jpedsurg.2012.08.037
Tran K, Kuo B, Zibaitis A, Bhattacharya S, Cote C, Belkind-Gerson J. Effect of propofol on anal sphincter pressure during anorectal manometry. J Pediatr Gastroenterol Nutr. 2014;58(4):495-497. https://doi.org/10.1097/MPG.0000000000000190
Sharma A, Herekar A, Yan Y, Karunaratne T, Rao SSC. Dyssynergic Defecation and Other Evacuation Disorders. Gastroenterol Clin North Am. 2022;51(1):55-69. https://doi.org/10.1016/j.gtc.2021.10.004
García-Valencia OA, Sánchez-Ávila MT, Martínez-Ordaz L, Hernández-Flores I, Moreno Medrano E, Morales-Garza LA, et al. Características manométricas en niños con estreñimiento crónico y patología anorrectal adquirida. Rev Gastroenterol Perú. 2019;39(2):136-140.
Zhao Y, Ren X, Qiao W, Dong L, He S, Yin Y. High-resolution Anorectal Manometry in the Diagnosis of Functional Defecation Disorder in Patients With Functional Constipation: A Retrospective Cohort Study. J Neurogastroenterol Motil. 2019;25(2):250-257. https://doi.org/10.5056/jnm18032
Alessandrella A, Turco R, Russo M, Poziello A, Miele E, Staiano A. High-resolution anorectal manometry in children with functional constipation with or without fecal incontinence. Neurogastroenterol Motil. 2020;32(9):e13882. https://doi.org/10.1111/nmo.13882
Fathy A, Megahed A, Barakat T, Abdalla AF. Anorectal functional abnormalities in Egyptian children with chronic functional constipation. Arab J Gastroenterol. 2013;14(1):6-9. https://doi.org/10.1016/j.ajg.2013.02.001
El-Shabrawi M, Hanafi HM, Abdelgawad MMAH, Hassanin F, Mahfouze AAA, Khalil AFM, et al. High-resolution anorectal manometry in children with functional constipation: a single-centre experience before and after treatment. Prz Gastroenterol. 2018;13(4):305-312. https://doi.org/10.5114/pg.2018.79810
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2024 Revista colombiana de Gastroenterología

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Aquellos autores/as que tengan publicaciones con esta revista, aceptan los términos siguientes:
Los autores/as ceden sus derechos de autor y garantizarán a la revista el derecho de primera publicación de su obra, el cuál estará simultáneamente sujeto a la Licencia de reconocimiento de Creative Commons que permite a terceros compartir la obra siempre que se indique su autor y su primera publicación en esta revista.
Los contenidos están protegidos bajo una licencia de Creative Commons Reconocimiento-NoComercial-SinObraDerivada 4.0 Internacional.



















