Fulminant Intestinal Amebiasis in a Young Female Patient: A Case Report
DOI:
https://doi.org/10.22516/25007440.1150Keywords:
Gastrointestinal bleeding, Hematochezia, Entamoeba histolytica, Amoebic dysentery, ColectomyAbstract
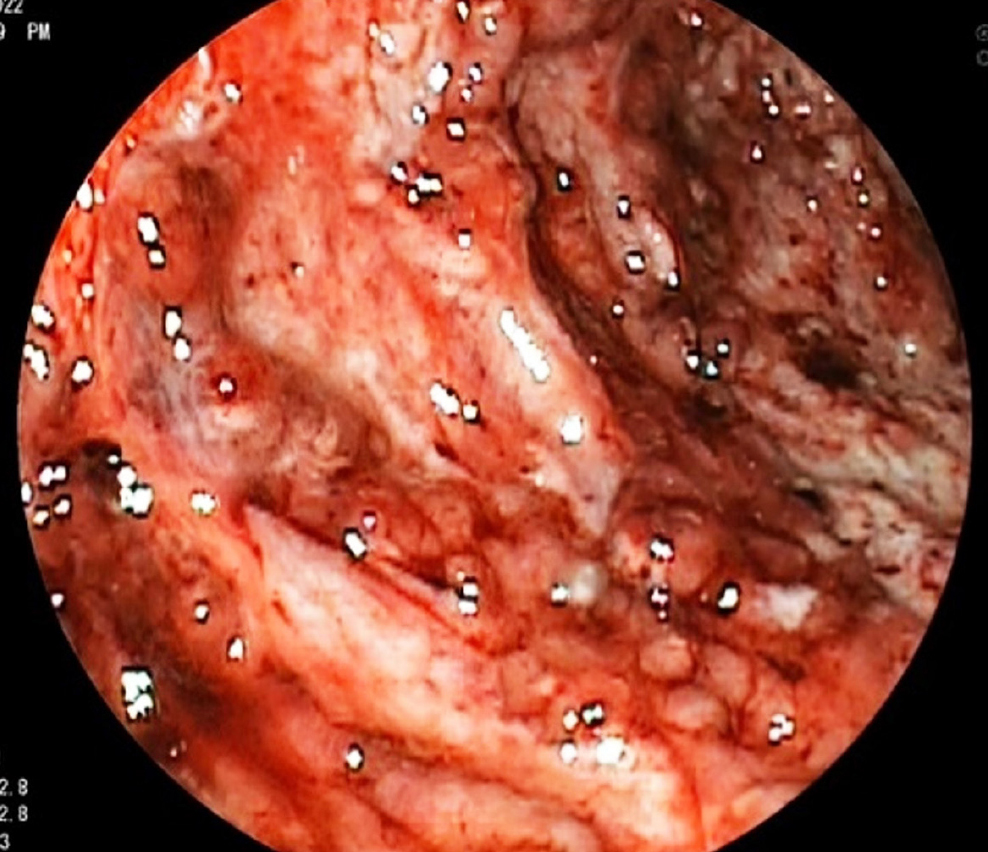
Intestinal amebiasis is an endemic disease in developing countries caused by the protozoan Entamoeba histolytica. It is typically asymptomatic, but in rare cases, it can present with severe manifestations. This is the case of a 30-year-old female patient who, two days after undergoing open appendectomy, developed rectal bleeding and abdominal pain accompanied by signs of hemodynamic instability. Colonoscopy revealed multiple necrotic ulcers in the mucosa with abundant clots. The patient experienced clinical deterioration, persistent bleeding, and signs of peritoneal irritation, necessitating exploratory laparotomy. Intraoperative findings included hypoperfused colon and cecal perforation, requiring total colectomy. Histopathological analysis confirmed acute severe ulcerative colitis caused by E. histolytica.
Downloads
References
Carrero JC, Reyes-López M, Serrano-Luna J, Shibayama M, Unzueta J, León-Sicairos N, et al. Intestinal amoebiasis: 160 years of its first detection and still remains as a health problem in developing countries. Int J Med Microbiol. 2020;310(1):151358. https://doi.org/10.1016/j.ijmm.2019.151358
Pinilla AE, López MC, Viasus DF. Historia del protozoo Entamoeba histolytica. Rev Méd Chile. 2008;136(1):118-24. https://doi.org/10.4067/S0034-98872008000100015
Kantor M, Abrantes A, Estevez A, Schiller A, Torrent J, Gascon J, et al. Entamoeba Histolytica: Updates in Clinical Manifestation, Pathogenesis, and Vaccine Development. Can J Gastroenterol Hepatol. 2018;2018:4601420. https://doi.org/10.1155/2018/4601420
Haque R, Huston CD, Hughes M, Houpt E, Petri WA. Amebiasis. N Engl J Med. 2003;348(16):1565-73. https://doi.org/10.1056/NEJMra022710
Qayed E, Dagar G, Nanchal RS. Lower Gastrointestinal Hemorrhage. Critical Care Clinics. 2016;32(2):241-54. https://doi.org/10.1016/j.ccc.2015.12.004
Gralnek IM, Neeman Z, Strate LL. Acute Lower Gastrointestinal Bleeding. N Engl J Med. 2017;376(11):1054-63. https://doi.org/10.1056/NEJMcp1603455
Hawks MK, Svarverud JE. Acute Lower Gastrointestinal Bleeding: Evaluation and Management. Am Fam Physician. 2020;101(4):206-212.
Whitehurst BD. Lower Gastrointestinal Bleeding. Surg Clin North Am. 2018;98(5):1059-72. https://doi.org/10.1016/j.suc.2018.06.007
Strate LL, Naumann CR. The Role of Colonoscopy and Radiological Procedures in the Management of Acute Lower Intestinal Bleeding. Clin Gastroenterol Hepatol. 2010;8(4):333-43. https://doi.org/10.1016/j.cgh.2009.12.017
Beck KR, Shergill AK. Colonoscopy in Acute Lower Gastrointestinal Bleeding. Gastrointestinal Endosc Clin North Am. 2018;28(3):379-90. https://doi.org/10.1016/j.giec.2018.02.009
Strate LL, Gralnek IM. ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding. Am J Gastroenterol. 2016;111(4):459-74. https://doi.org/10.1038/ajg.2016.41
Oakland K, Chadwick G, East JE, Guy R, Humphries A, Jairath V, et al. Diagnosis and management of acute lower gastrointestinal bleeding: guidelines from the British Society of Gastroenterology. Gut. 2019;68(5):776-89. https://doi.org/10.1136/gutjnl-2018-317807
Iqbal T, DuPont HL. Approach to the patient with infectious colitis: clinical features, work-up and treatment. Curr Opin Gastroenterol. 2021;37(1):66-75. https://doi.org/10.1097/MOG.0000000000000693
Thielman NM, Guerrant RL. Clinical practice. Acute infectious diarrhea. N Engl J Med. 2004;350(1):38-47. https://doi.org/10.1056/NEJMcp031534
Beg MY, Bains L, Mahajan R, Lal P, Choudhury S, Kumar NP, et al. Fulminant Necrotising Amoebic Colitis of Whole of Large Bowel: A Rare Complication of a Common Infectious Disease. Case Rep Infect Dis. 2020;2020:8845263. https://doi.org/10.1155/2020/8845263
Jessurun J. The Differential Diagnosis of Acute Colitis: Clues to a Specific Diagnosis. Surg Pathol Clin. 2017;10(4):863-85. https://doi.org/10.1016/j.path.2017.07.008
Uddin MJ, Leslie JL, Petri WA. Host Protective Mechanisms to Intestinal Amebiasis. Trends Parasitol. 2021;37(2):165-75. https://doi.org/10.1016/j.pt.2020.09.015
Petri WA, Smith RD, Schlesinger PH, Murphy CF, Ravdin JI. Isolation of the galactose-binding lectin that mediates the in vitro adherence of Entamoeba histolytica. J Clin Invest. 1987;80(5):1238-44. https://doi.org/10.1172/JCI113198
Begum S, Quach J, Chadee K. Immune Evasion Mechanisms of Entamoeba histolytica: Progression to Disease. Front Microbiol. 2015;6:1394. https://doi.org/10.3389/fmicb.2015.01394
Ralston KS, Solga MD, Mackey-Lawrence NM, Somlata, Bhattacharya A, Petri WA Jr. Trogocytosis by Entamoeba histolytica contributes to cell killing and tissue invasion. Nature. 2014;508(7497):526-30. https://doi.org/10.1038/nature13242
Ito D, Hata S, Seiichiro S, Kobayashi K, Teruya M, Kaminishi M. Amebiasis presenting as acute appendicitis: Report of a case and review of Japanese literature. Int J Surg Case Rep. 2014;5(12):1054-7. https://doi.org/10.1016/j.ijscr.2014.10.035
Otan E, Akbulut S, Kayaalp C. Amebic Acute Appendicitis: Systematic Review of 174 Cases. World J Surg. 2013;37(9):2061-73. https://doi.org/10.1007/s00268-013-2079-5
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2024 Revista colombiana de Gastroenterología

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Aquellos autores/as que tengan publicaciones con esta revista, aceptan los términos siguientes:
Los autores/as ceden sus derechos de autor y garantizarán a la revista el derecho de primera publicación de su obra, el cuál estará simultáneamente sujeto a la Licencia de reconocimiento de Creative Commons que permite a terceros compartir la obra siempre que se indique su autor y su primera publicación en esta revista.
Los contenidos están protegidos bajo una licencia de Creative Commons Reconocimiento-NoComercial-SinObraDerivada 4.0 Internacional.



















