Atypical Intestinal Lesions in a Patient with Neurofibromatosis Type 1: A Case Report
DOI:
https://doi.org/10.22516/25007440.1114Keywords:
Neurofibromatosis, Neurofibroma, Gastrointestinal stromal tumor, Atypical intestinal lesionsAbstract
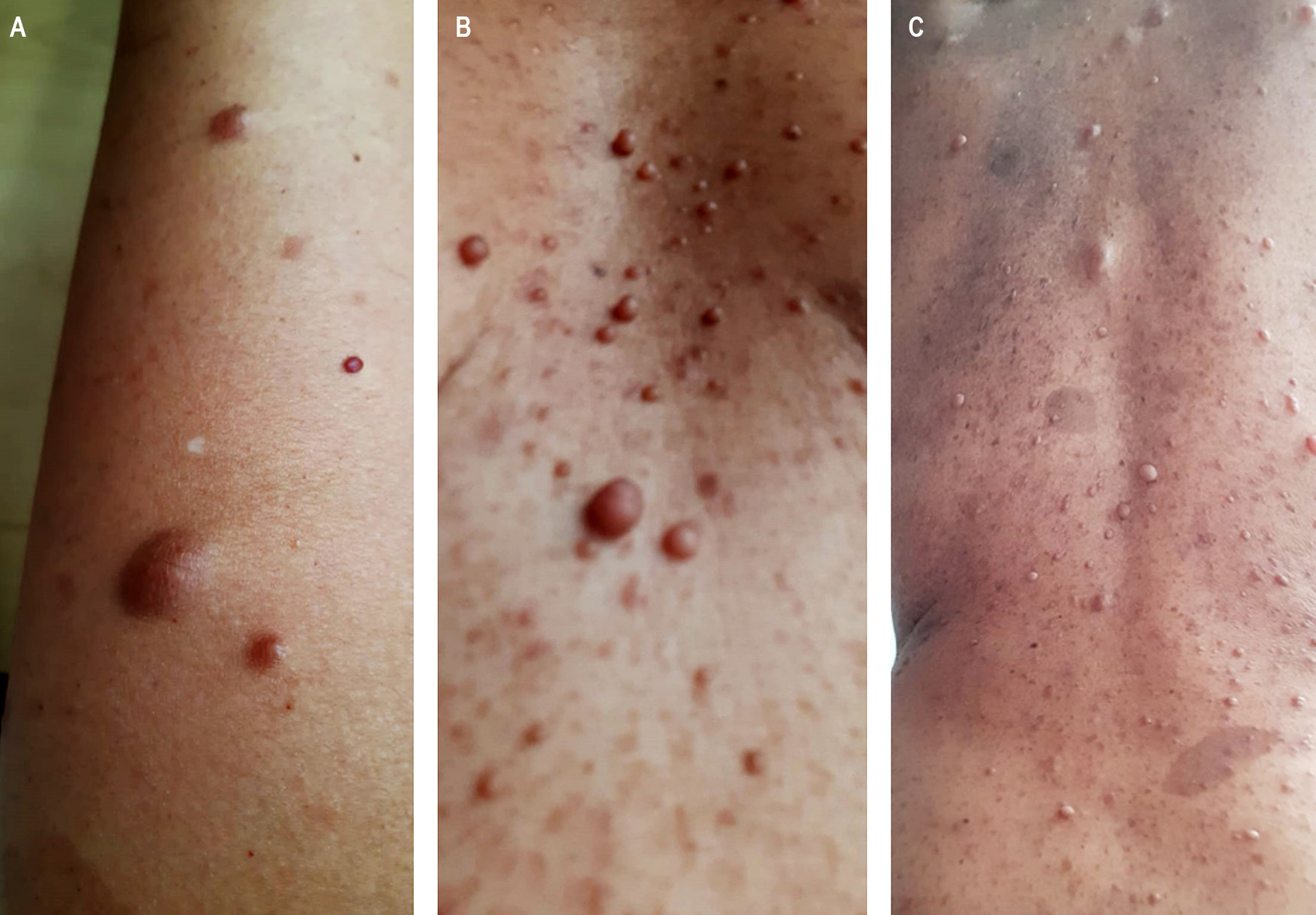
Neurofibromatosis type 1 (NF1) is a neurocutaneous disorder that can manifest as multiple tumors or plexiform lesions in the gastrointestinal tract and extraintestinal sites. Gastrointestinal involvement occurs in 10%–25% of patients, with neurofibromas being the most common lesions, typically located in the small intestine. When multiple tumors are found in the small intestine, they are often gastrointestinal stromal tumors (GISTs). This case report presents a 55-year-old woman with a history of NF1, characterized by neurofibromas and café-au-lait spots across her body. She was evaluated as an outpatient in the endoscopy unit at Unión de Cirujanos S. A. S. in Manizales, Colombia, within the Gastroenterology Surgical Clinic Service at Universidad de Caldas. The patient underwent ileocolonoscopy after a positive fecal occult blood test. She denied abdominal pain, hematochezia, rectal bleeding, or melena. Ileocolonoscopy revealed nodular lesions ranging from 3 to 5 mm in the distal ileum. Endoscopic resection was performed on one lesion, which was sent for histopathological examination.
Downloads
References
Kijima T, Ishida S, Kishi T, Yamaguchi M. Bowel intussusception and adhesive intestinal obstruction in neurofibromatosis type 1. J Gen Fam Med. 2022;23(5):354-355. https://doi.org/10.1002/jgf2.547
Garrouche N, Ben Abdallah A, Arifa N, Hasni I, Ben Cheikh Y, Ben Farhat W, et al. Spectrum of gastrointestinal lesions of neurofibromatosis type 1: a pictorial review. Insights Imaging. 2018;9(5):661-671. https://doi.org/10.1007/s13244-018-0648-8
Gamarra ER, Ruiz PD. Gastrointestinal hemorrhage due to neurofibromatosis type 1: a case report. Horiz Med (Lima). 2020;20(4):e1412.
Selfa-Muñoz A, Ruiz-Escolano E, Martínez-Tirado P, López-Segura Rdel P, Sáez-Zafra A, Salmerón-Escobar FJ. Hemorragia digestiva secundaria a neurofibromatosis intestinal. Rev Esp Enferm Dig (Madrid) 2012;104(2):99-100. https://doi.org/10.4321/S1130-01082012000200012
Zulfiqar M, Lin M, Ratkowski K, Gagnon MH, Menias C, Siegel CL. Imaging Features of Neurofibromatosis Type 1 in the Abdomen and Pelvis. AJR Am J Roentgenol. 2021;216(1):241-251. https://doi.org/10.2214/AJR.19.22283
Méndez D, Oricchio M, Pontet Y, Otero M, Muñiz F, Cubas S, et al. Manifestaciones gastrointestinales en neurofibromatosis tipo 1. Reporte de un caso. Acta Gastroenterol Latinoam. 2020;50(4):474-478. https://doi.org/10.52787/GKNO4993
Pontone S, Cicerone C, Magliocca FM, Pironi D, Sorrenti S, Filippini A, et al. Intestinal neurofibromatosis found on surveillance colonoscopy. Tech Coloproctol. 2017;21(2):171-174. https://doi.org/10.1007/s10151-017-1588-x
Dare AJ, Gupta AA, Thipphavong S, Miettinen M, Gladdy RA. Abdominal neoplastic manifestations of neurofibromatosis type 1. Neurooncol Adv. 2020;2(Suppl 1):i124-i133. https://doi.org/10.1093/noajnl/vdaa032
Mishra A, Gyawali S, Kharel S, Mishra A, Pathak N, Subedi N, et al. Multiple jejunal gastrointestinal stromal tumors and Neurofibromatosis type 1: A rare association. Int J Surg Case Rep. 2021;85:106178. https://doi.org/10.1016/j.ijscr.2021.106178
Yao MQ, Jiang YP, Yi BH, Yang Y, Sun DZ, Fan JX. Neurofibromatosis type 1 with multiple gastrointestinal stromal tumors: A case report. World J Clin Cases. 2023;11(10):2336-2342. https://doi.org/10.12998/wjcc.v11.i10.2336
Flores Delgado EA, Flores Miranda E. Neurofibroma del mesenterio en un paciente sin enfermedad de Von Recklinghausen. Rev Cubana Cir. 2016;55(4):325-333.
Ahn S, Chung CS, Kim KM. Neurofibroma of the Colon: A Diagnostic Mimicker of Gastrointestinal Stromal Tumor. Case Rep Gastroenterol 2016;10(3):674-678. https://doi.org/10.1159/000452202
Ríos C, Mora GA. Neurofibromatosis tipo 1 - Enfermedad de Von Recklinghausen. Revista Médica de Costa Rica y Centroamérica. 2014;71(610):249-252.
Gómez MA, Lúquez AJ. Neurofibromatosis tipo 1 y sangrado de intestino delgado. Rev Fac Med. 2017;65(4):683-685. https://doi.org/10.15446/revfacmed.v65n4.59619
Guldfeldt P, Zardari R. Small Bowel Obstruction Due to Gastrointestinal Neurofibromas and Lipomas. J Med Cases. 2014;5(1):1-3. https://doi.org/10.4021/jmc1579w
Arango Molano LA, Díaz CP, Londoño M, Ortiz Restrepo P, Cano Méndez LM. Lipomatosis intestinal: reporte de dos casos. Rev Colomb Gastroenterol. 2020;35(2):212-5. https://doi.org/10.22516/25007440.288
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2024 Revista colombiana de Gastroenterología

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Aquellos autores/as que tengan publicaciones con esta revista, aceptan los términos siguientes:
Los autores/as ceden sus derechos de autor y garantizarán a la revista el derecho de primera publicación de su obra, el cuál estará simultáneamente sujeto a la Licencia de reconocimiento de Creative Commons que permite a terceros compartir la obra siempre que se indique su autor y su primera publicación en esta revista.
Los contenidos están protegidos bajo una licencia de Creative Commons Reconocimiento-NoComercial-SinObraDerivada 4.0 Internacional.



















